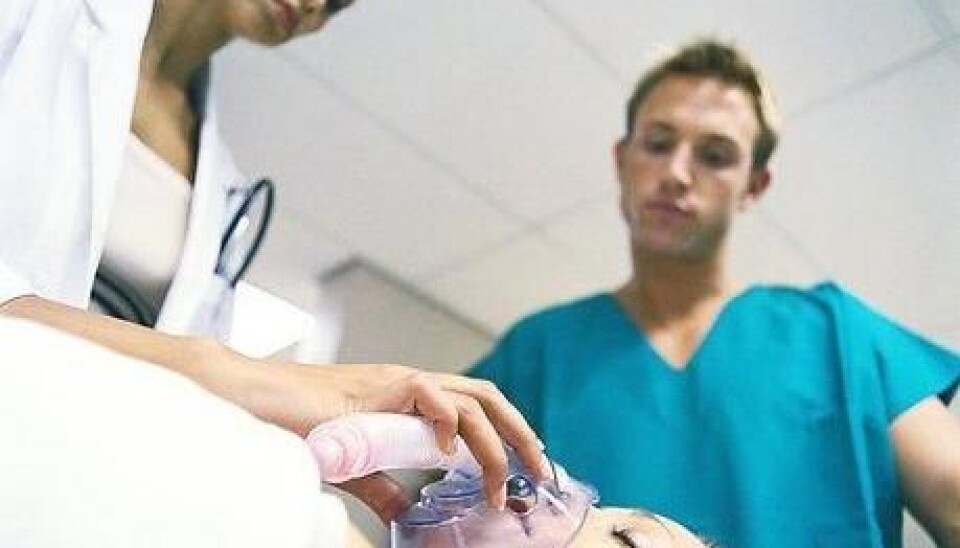
Artificial comas can cause kidney failure
Inducing a patient into an artificial coma can end with kidney failure, making the patient’s condition even worse. This practice should be changed, says researcher.
New research shows that an artificial or induced coma damages the patient’s health in the long term and can lead to kidney failure and other diseases.
As a result, a Danish researcher wants to change what has become routine use of induced comas.
“A patient with renal failure – when the kidneys stop working – is in a really bad situation,” says Thomas Strøm, PhD, a clinical associate professor in anaesthesiology at the University of Southern Denmark, who led a team that examined several factors among hospitalised patients.
“We can see that an induced coma can give a patient a poorer physical condition than he or she would have otherwise had. The use of induced comas as a standard treatment must be changed.”
Whole body is anaesthetised
Placing patients in an artificial coma means that not only the brain but the whole body is anaesthetised. As a result, patients in induced comas often experience many complications resulting from the comprehensive medical treatment involved in an artificial coma.
Strøm and his colleagues examined a number of medical parameters, including urine volume, blood pressure and circulation of patients in induced coma and patients treated in a respirator, but not in induced coma.
“We can see that avoiding the use of induced coma when the patient is in a respirator is beneficial,” says Strøm.
“Our results show fewer cases of renal failure – and they support the theory that being placed in an artificial coma is a great strain on the body.”
Shorter stay in hospital
In 2010, the same research team managed to document that the time patients are in hospital can be cut if doctors don’t use induced comas when patients are given respirator treatment.
That study was published in the medical journal The Lancet and it resulted in changes to the national guidelines for induced comas and respirator treatment. Later there were recommendations to limit the use of artificial comas.
No psychological injuries
In connection with the 2010 study, many researchers feared that patients would suffer psychologically because they were conscious and in a respirator at the same time.
“Questions were raised about whether patients had become nervous wrecks and if it would not be more psychologically beneficial if the patients were in an artificial coma during their respirator treatment,” says Strøm.
“We asked a psychologist to assess the patients after their treatment, and I can say that being conscious while in the respirator did not add to their stress.”
Strøm continues his work by examining the benefits for critically ill patients if they are not in an induced coma during respirator treatment.
------------------------------
Read this story in Danish at videnskab.dk
Translated by: Michael de Laine
Scientific links
- A protocol of no sedation for critically ill patients receiving mechanical ventilation: a randomised trial, The Lancet, doi:10.1016/S0140-6736(09)62072-9
- Sedation and renal impairment in critically ill patients: a post hoc analysis of a randomized trial, Critical Care, doi:10.1186/cc10218
- Long-term psychological effects of a no-sedation protocol in critically ill patients, Critical Care, doi:10.1186/cc10586






