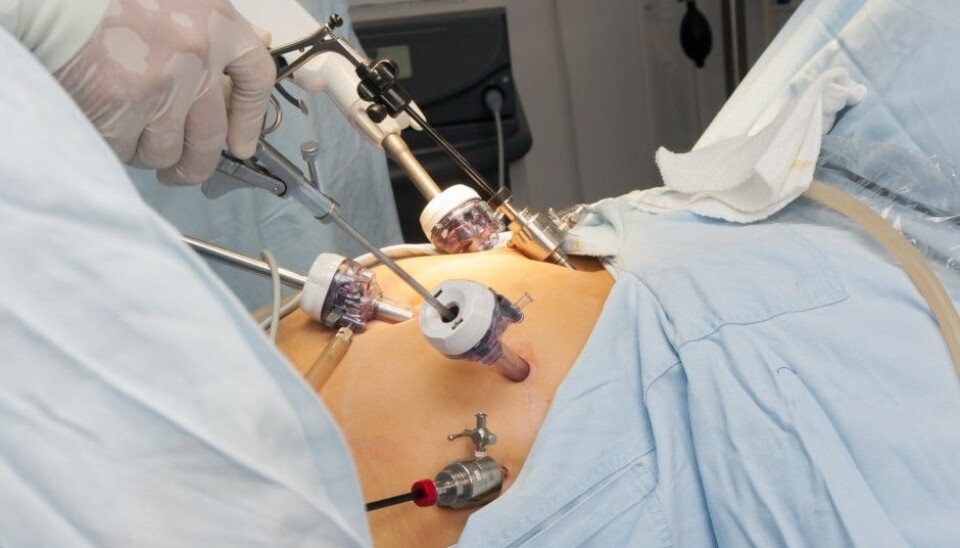
Why some experience serious side effects from bariatric surgery
What happens during bariatric surgery can be just as important as the health of the patient before the operation takes place.
Serious side effects after bariatric surgery can largely be blamed on the surgery itself, and not so much on the patient’s condition, according to Erik Stenberg, who has studied the operation and its aftermath as part of his PhD dissertation at Örebro University in Sweden.
“Often, the focus is on factors involving the patient,” he said in an email. “Some of these factors are important, of course, but what happens during the operation has even greater significance.”
Stenberg has focused his research on the more serious consequences of bariatric surgery, such as bleeding or leakage, and not on the usual problems facing those who have the operation, such as diarrhoea or fatigue.
He found that the highest risk of serious complications results when something goes wrong during the surgery, or if the surgeon has to shift from keyhole surgery to open surgery.
Stenberg’s research suggests that the operation itself appears to have greater significance than the patient's weight, sex and pre-existing illnesses.
Experienced surgeons reduce risks
Hospitals that have done at least 400 of this kind of surgery and at a rate of least 200 operations per year increase the likelihood that the operation will go well, Stenberg found.
The Norwegian obesity researcher Jøran Hjelmesæth is impressed with the quality of the Swedish study, but does not totally agree that the operation is more important than the patient in determining the outcome of the surgery.
“Both are important,” says Hjelmesæth, a professor at the University of Oslo and head of the Centre for Morbid Obesity at Vestfold Hospital.
Some conditions do increase risks
In spite of his assertion on the significance of the operation itself, Stenberg nevertheless believes it is important to be aware that some types of patients run a greater risk of complications during surgery.
Other studies have shown that a very high body mass index (BMI) is associated with an increased risk of complications. Men are also more susceptible. Stenberg found, however, that high blood sugar and age are the two most important factors that increase the risk of post-operative side effects.
Hjelmesæth suggests that Stenberg’s findings may be due to the fact that surgeons will be cautious about operating on an elderly man who has a very high BMI and diabetes. That means these patients are probably less likely to end up in a register of side effects from bariatric surgery, which is what the Swedish study is based on.
Preventing a serious side effect
Stenberg studied the type of bariatric surgery that is most common in both Sweden and Norway, called gastric bypass surgery.
This is done using keyhole surgery and is considered safe. Nevertheless, it can still cause some potentially serious side effects, ranging from leaks to bleeding.
Volvulus, or a twist in the gut, is one such complication. This is when the small intestine twists so much that the bowel is obstructed. The condition is both painful and very serious.
Much of the bowel is attached to a kind of curtain, called the mesentery, which in turn is attached to the abdominal cavity. During gastric bypass surgery, the surgeon shortens the bowel, and attaches the two remaining parts of the small intestine to each other. The mesentery at this location will have small openings in it, called slits.
The intestine can become lodged in these openings and be pinched, causing volvulus. In this situation, patients will end up back on the operating table again.
But if the slits in the mesentery are closed, the risk of a patient having to return to the operating table again within three years after bariatric surgery was halved, from about 10 to 5 per cent.
This is what Stenberg found when he compared two groups in a randomized, controlled trial.
Higher short-term risk when openings are closed
However, Stenberg found that closing the slits had a slightly higher risk of volvulus right after surgery, with an increase from just under 3 to a little over 4 per cent.
Stenberg still recommends that surgeons close the slits, a recommendation supported by Jon Kristinsson at Oslo University Hospital (OUS).
“We believe that the rewards are so great from closing the slits that we accept some increased risk of complications over the short term,” Kristinsson said.
Kristinsson says that his hospital and the Department of Morbid Obesity and Bariatric Surgery, which he leads, had already switched over to this approach seven or eight years ago. They were inspired by the private hospital Aleris, which followed up on their patients and found that there was less volvulus over the long term after surgeons began to close the slits in the mesentery.
Hjelmesæth believes, however, that while Stenberg’s work is valuable, the field needs at least one more study before researchers can say that closing the slits in the mesentery should be standard practice. Researchers do not yet know why patients face an increased risk of volvulus right after surgery, he said.
--------------------------------------
Read the Norwegian version of this article at forskning.no