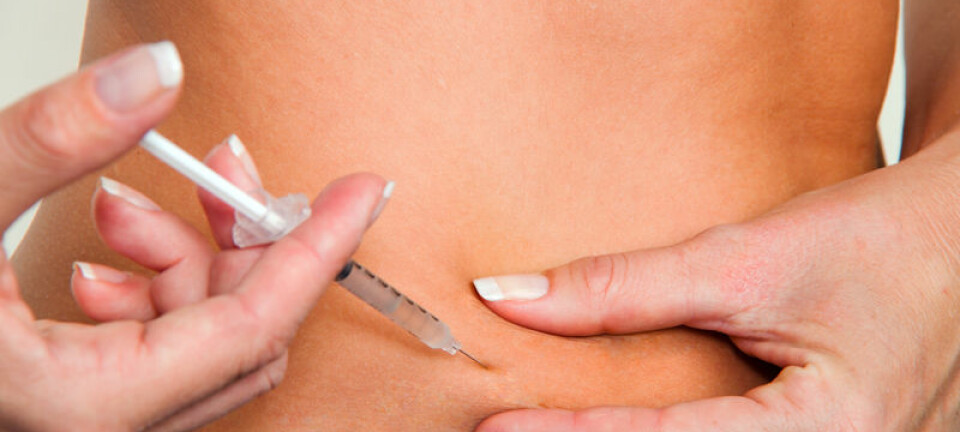
Slim and healthy people also get type 2 diabetes
Researchers have found a way of dividing type 2 diabetes patients into subgroups. Surprisingly, only one in four patients goes through what is considered the most common course of the disease.
Overweight, an unhealthy lifestyle and old age are factors that many of us associate with people who are diagnosed with type 2 diabetes.
But this isn’t entirely true. In fact, the disease can hit the slim, the fat, the young and the old.
This diversity of patients does not make life easy for doctors and researchers, as it creates a need for a great variety of treatment forms. For example, lifestyle changes only work for some patients and not for others. The ideal time for an insulin fix also varies greatly, depending on the patient.
However, now two Danish researchers have cracked part of this code. Based on data from a comprehensive English study, they have identified three subgroups of type 2 diabetes patients that have different diseases patterns.
It was previously believed that the most common course for diabetes is that the patient first develops insulin resistance – which means that the effectiveness of the insulin is reduced. To compensate, the beta cells in the body produce more and more insulin.
In addition to showing that diabetes is expressed in a variety of ways, the study surprises by showing that only 25 percent of the type 2 diabetes patients follow the course of the disease that scientists so far have considered to be the most common one.
”This finding is the first step towards more targeted prevention and treatment for patients with the different subgroups of the disease,” says Kristine Færch, a senior researcher at the Steno Diabetes Center, who co-authored the study.
Classification determined by blood sugar
Insulin is the key ingredient when we’re talking about type 2 diabetes. Insulin is produced in the body and works by transporting the energy from our food into the cells, where the energy is used.
Type 2 diabetes occurs either:
- As a result of insulin resistance, where the insulin gradually loses its ability to transport energy from food to the muscles.
- As a result of problems with the beta cells, which are those that produce or secrete insulin.
At some point, the body cannot continue to produce more insulin, and then the insulin production decreases. Somewhere in this process the blood sugar levels start to rise. This course has been regarded as the prevalent type of type 2 diabetes, but now we have discovered that this course only applies to 25 percent of those who get type 2 diabetes.
The interaction between insulin resistance and beta-cell function is important for maintaining stable blood sugar levels. Insulin resistance and problems with the beta cells cause high blood sugar, also known as hyperglycemia.
High blood sugar manifests itself in the short term through symptoms such as nausea, thirst and fatigue, while in the long term it can damage the blood vessels.
Diagnosis of diabetes
A doctor can determine whether a person has diabetes by measuring the following:
- The person’s blood sugar levels after an overnight fast.
- The person’s blood sugar levels after taking a so-called glucose load, consisting of a dose of glucose solution.
- The person’s long-term hyperglycemia, also known as haemoglobin A1C (HbA1c).
- The person’s blood sugar levels at any time of the day (if the person is displaying symptoms of diabetes).
Three subgroups of patients
It is likely that the groups would benefit from a variety of treatment forms. If they respond differently to drugs, the subgroups will benefit from different types of prevention, and so on.
The Danish researchers then created three subgroups based on the patients’ blood sugar levels in the first two of the tests mentioned above.
- The first group has high blood sugar after fasting and after taking a glucose load and makes up around 25 percent of patients.
- The second group has high blood sugar after fasting, but not after taking a glucose load and accounts for around 20 percent of patients.
- The third group has high blood sugar after taking a glucose load, but not after fasting. This group is by far the largest, representing about 55 percent.
Group 1: only 25 percent have ‘typical’ course
One of the surprising conclusions in the study is that only one in four of the participants who had high blood sugar after both fasting and receiving a glucose load had a development of beta cell function similar to what has so far been considered as a ‘normal’ course.
“It was previously believed that the most common course for diabetes is that the patient first develops insulin resistance – which means that the effectiveness of the insulin is reduced. To compensate, the beta cells in the body produce more and more insulin,” says Færch.
“At some point, the body cannot continue to produce more insulin, and then the insulin production decreases. Somewhere in this process the blood sugar levels start to rise. This course has been regarded as the prevalent type of type 2 diabetes, but now we have discovered that this course only applies to 25 percent of those who get type 2 diabetes.”
The researchers also found that these 25 percent have a greater risk of suffering from cardiovascular disease than patients in the other two subgroups.
“It is therefore important that future studies look at whether the increased risk in this group is also reflected in an increased incidence of cardiovascular disease, and if so, whether it makes sense to increase the efforts to prevent cardiovascular disease in a more targeted way for these 25 percent,” says Færch.
Group 2: possibly a congenital defect
The second group, which had high blood sugar after fasting but not after a glucose load, turned out to have insufficient insulin secretion throughout the 18-year period covered by the study.
This caused slightly elevated blood sugar levels in during fasting and is associated with low beta-cell function. Beta cells are the cells responsible for the production and secretion of insulin.
”There are indications that this group has a congenital defect in their insulin secretion, which may contribute to the development of diabetes later on in life.”
According to the researcher, this suggests that this subgroup of diabetes patients may be more genetically predisposed than the first group, where lifestyle probably plays a greater part.
”The first group typically consists of highly overweight people – even many years before they are diagnosed with diabetes – while the second and third groups are nearer to the average body weight,” she says.
This could have an impact on how the various groups should be treated, since other studies have shown that lifestyle changes work well for patients who fall into the first group, while they have less of an effect on patients in group 2.
On the other hand, it may be relevant to put group 2 patients into treatment with insulin or other diabetes drugs at an earlier stage than they normally would.
Group 3: normal beta cells
In group 3, which counts more than half of the participants, the researchers observed normal insulin secretion throughout the 18-year period. These patients’ beta cells function as they should, in contrast to groups 1 and 2.
“This indicates that it’s the effectiveness of their insulin that is reduced over the years – they become insulin resistant. This is often associated with inactivity, but this group is not as overweight as group 1,” says Færch.
Basis for further studies
In the longer term, the classification of diabetes patients into subgroups could lead to improved treatment. But further studies are needed.
First of all, the findings from this study need to be reviewed by other researchers, but it’s also relevant to use the new findings to look at whether patients from different subgroups also respond differently to treatment after being diagnosed with diabetes.
”It is likely that the groups would benefit from a variety of treatment forms. If they respond differently to drugs, the subgroups will benefit from different types of prevention, and so on.”
-------------------------
Read the Danish version of this article at videnskab.dk
Translated by: Dann Vinther