HIV epidemic in Greenland mapped in great detail
HIV has been introduced in Greenland at least 25 times, according to new study, which reveals how an HIV epidemic breaks out and spreads in a society. The findings may help prevent future epidemics.
Danish and Swedish scientists have mapped the origin and spread of HIV in Greenland in stunning, patient-level detail. This is the first time an HIV epidemic has been studied in such detail, and the new study provides a model for understanding how HIV has spread globally, as well as offering suggestions on how to prevent future epidemics.
“The HIV/AIDS epidemic is a big problem, and it is very important to understand the dynamics of the epidemic,” says Christian Bruhn, a PhD fellow at the Center for Geogenetics at the University of Copenhagen.
”Research-wise, it is pretty amazing and unique to have a dataset from which you can extract the entire history of an epidemic – including where from where and when the single epidemic introduction arrived in the country, how it spread and how many times HIV has been introduced in Greenland.”
Bruhn regards the study as a model for how HIV may have emerged globally, and how local outbreaks continue to occur. The study forms part of Bruhn’s PhD thesis, and is published in the journal AIDS.
Solid dataset
A few years ago, he and his supervisor, Professor Tom Gilbert, realised that Greenland is ideal for studying the mystery of how and why HIV epidemics occur.
This is partly due to the country’s small population of around 55,000 inhabitants and its geographical isolation, and also to a great extent because the Danish health registers and intensive local efforts in Greenland have resulted in a solid dataset with blood samples, genetic sequences of viruses and even patient interviews in which doctors traced the viruses back along the chain of infection.
“Not many datasets include data about when a chain of infection started and specific infection dates that identify who started the epidemic,” says Bruhn.
This means that it is possible to follow the epidemic up close from one patient to another, enabling the researchers to see e.g. whether it is predominantly biological or social factors that cause HIV to take hold and become an epidemic.
HIV introduced at least 25 times in Greenland
Not many datasets include data about when a chain of infection started and specific infection dates that identify who started the epidemic.
The researchers combined genetic family trees for the virus with classic epidemiological tools.
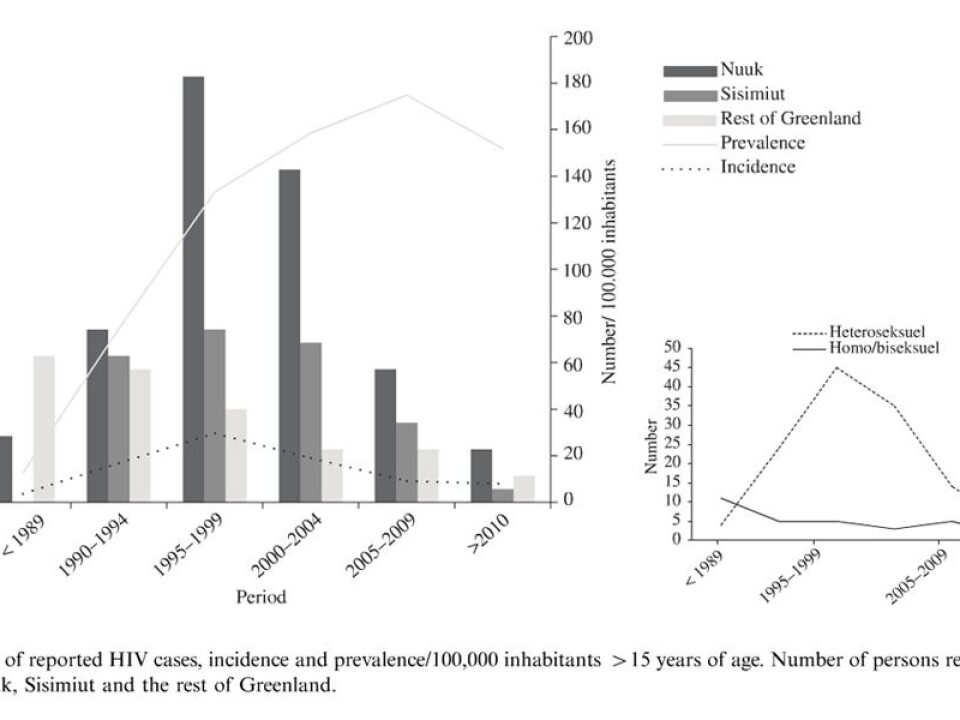
In Greenland, 174 people have been infected since the first case in 1985. When the researchers analysed the genetic relationship between 98 of these patients, they made a surprising discovery.
The results of the genetic sequencing revealed that while the HIV viruses are closely related, collectively they reveal that HIV has found its way to Greenland no less than 17 times.
When this figure is extrapolated to all 174 patients, the researchers estimate that HIV has been introduced at least 25 times in Greenland. In other words, surprisingly many HIV introductions have occurred at intervals over the past decades.
A single introduction dominates
It will be possible to see if a particular virus suddenly gains ground and manages to reach a new group in society, and this may help us to prevent an epidemic.
But the surprises do not stop there. Of all the introductions of HIV into Greenland, there has been a single one that was completely dominant and was responsible for a full 72 of the 98 HIV sequenced patients featured in the study. The remaining introductions led to either highly limited or no further infection.
This is surprising as one might expect a more even distribution of the various introductions of HIV, and this reveals that the HIV virus does not easily take hold in a population.
“However, this fits in neatly with the global picture in which individual subtypes dominate large regions such as the US, Europe and southern Africa,” says Bruhn.
”In the individual countries, we also see certain subtypes dominating various demographic groups.”
This obviously raises the question of why a certain HIV virus becomes a ’success’. Is it something biological such as a mutation that makes a certain virus particularly infectious, or is it due to other, perhaps social, factors?
HIV came from Denmark
The Nordic researchers can now answer this question in relation to the particularly ’successful’ HIV introduction in Greenland.
With their molecular sequence data, they can eliminate biological factors with relative ease, since the virus does not differ much from the other subtypes in the study.
However, having studied how the virus made its way into the community, they came across something interesting:
From homosexual to heterosexual transmission and from township to town
With the viral family tree, they could trace the origin to a small village in the mid-1980s and a Greenlandic man, who was homosexually infected in Denmark. After a few initial transfers of the virus through homosexual contact, the spread quickly changed character and became heterosexually transmitted.
This is crucial, as it opens a gateway to many more potential hosts. Around 1989, the virus took another decisive leap when a woman from the township infected a man with ties to Greenland’s cities, including Sisimiut and the captital, Nuuk.
In this way, the virus has continuously managed to find new openings to larger and larger audiences.
Prevention works – except for the lower rungs of society
When the epidemic introduction reached the main towns, several other HIV introductions had already arrived. Local doctors were on high alert because Greenland back then had some of the world’s highest rates of sexually transmitted diseases such as gonorrhoea.
The doctors anticipated a full-blown disaster, and this prompted an intensive prevention campaign.
Nevertheless, this one HIV introduction managed to evade the preventive efforts and continued to infect new people. This looked like a mystery, but it turned out that the virus had continued its string of ‘lucky’ transfers, as this time it had found its way to a social group outside the scope of the prevention campaign: the socially excluded.
In their study, Bruhn and his colleagues observed that around 1989, the newly-arrived HIV virus found its way to a group of unemployed, poor, alcoholic, homeless Greenlanders, who had become partly isolated from the rest of society.
”A good guess is that this group had simply been slow to embrace the precautions for safe sex,” says Bruhn.
Important barriers for HIV prevention
The new study thus paints a picture of a virus, which basically had a hard time establishing itself as an epidemic, but when a series of social and demographic factors fell into place, it turned out to be possible.
This insight may be crucial in the future prevention of epidemics. Although scientists now have a detailed molecular understanding of HIV and are working flat out to fight it, the virus is still alive and kicking.
New virus outbreaks occur all the time, and viruses find ways to new environments in society. In this sense, the sudden spread in Greenland in the mid-1980s is similar to what is seen today at the local level around the world.
Monitoring bottlenecks
The new study indicates that there are bottlenecks that the virus needs to pass through in order to establish an epidemic:
- The journey from Denmark to Greenland
- The shift between risk/infection groups
- The introduction into larger urban areas
- The point when the virus reached a social group at the lower rungs of society.
“If we can identify these bottlenecks and squeeze them shut, that would be a good place to start,” says Bruhn.
Sometimes only a few people connect two groups in society, and Bruhn believes that genetic family tree analyses of the viruses may prove to be an important tool in the preventive work.
”It will be possible to see if a particular virus suddenly gains ground and manages to reach a new group in society, and this may help us to prevent an epidemic.”
------------------
Read the Danish version of this article at videnskab.dk
Translated by: Dann Vinther
Scientific links
- "The origin and emergence of an HIV-1 epidemic: from introduction to endemicity", AIDS (2014), PMID: 24451158
- "The HIV epidemic in Greenland – a slow spreading infection among adult heterosexual Greenlanders", International Journal of Circumpolar Health (2013), DOI: 10.3402/ijch.v72i0.19558